Delivery service
Free Worldwide Shipping & Returns
Free Worldwide Shipping & Returns
40% Discount for you
Tax Free Shopping
80,000+ Satisfied Customers
 Aquayer Plan Stop 5 tablets
Aquayer Plan Stop 5 tablets
 Tetra Med G-Tonic 20ml
Tetra Med G-Tonic 20ml
 Sera med Professional Nema 10 ml
Sera med Professional Nema 10 ml
 Sera med Professional Trema 25 ml
Sera med Professional Trema 25 ml
 Veterinary needle single 20G×1 ″, 0.9×25 mm 200 pcs
Veterinary needle single 20G×1 ″, 0.9×25 mm 200 pcs
 Hobby Viras 200ml (6.76oz)
Hobby Viras 200ml (6.76oz)
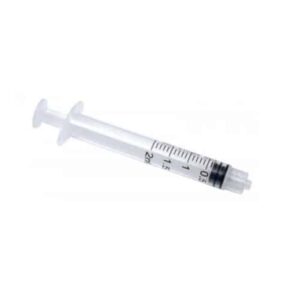 Disposable syringe 2 ml Luer Lock needle 0.6x25 mm Medicare, 100 pcs
Disposable syringe 2 ml Luer Lock needle 0.6x25 mm Medicare, 100 pcs
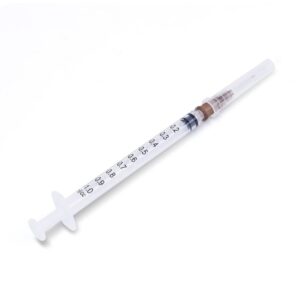 Disposable syringe 1 ml Alexpharm needle of 0,3х13 mm * 100 pcs
Disposable syringe 1 ml Alexpharm needle of 0,3х13 mm * 100 pcs
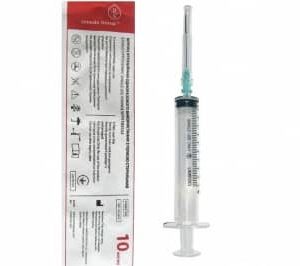 Disposable syringe 10 ml Luer Slip needle 0.8×38 mm Medicare, 100 pcs
Disposable syringe 10 ml Luer Slip needle 0.8×38 mm Medicare, 100 pcs
Farm animals — domestic animals kept by humans for food (meat, milk, eggs), fat, raw materials (wool, fur, down), bristles, skin, bones, feathers), as well as performing transport and working functions (traction, pack animals); bred by selection — selection of the desired qualities and characteristics of wild nature, since ancient times captured and tamed birds and animals.
Lamb
The term “Farm animals” usually includes various species and breeds of mammals, birds, fish and other aquatic animals, as well as insects kept in specialized non-residential premises in order to obtain primarily the products of life from representatives of bred animals.
Farm animals are most often kept in specialized non-residential premises (stables, corrals, sheds, stables, pigsties, cowsheds, rabbit houses, livestock buildings, farms, barns, barnyards, poultry houses, apiaries, and so on).
farm animals include:
livestock,
valuable fur-bearing animals,
rabbits,
birds,
and bees.
Farm animals are included in the General biological classification along with their wild relatives and at the same time are divided by breed.
List of farm animals
Mammals
Artiodactyls
Cattle
cows, buffaloes, bantengs, gayals, yaks, and their hybrids
Small cattle
goats, sheep
pigs
reindeer
camels: DROMEDARY (one-humped) and Bactrian (two-humped); llamas, Alpaca
Ungulate horses, donkeys, and their hybrids: mules and mules
Hare
like rabbits
Rodents
nutria
chinchillas
Guinea pigs
Predatory
Sables, European Minks, ferrets ,
dogs, foxes
Birds
Chicken, pheasant, quail, peacock
Guinea fowl
Geese-like
geese
ducks, musk ducks
Pigeon-like
pigeons (meat breeds)
Ostrich-like
Ostriches
Actinopterygii
Asociarse
Atlantic salmon, rainbow trout
Carp
like white cupids, white and variegated silver carp, carp, crucian carp, etc.
Insects
Hymenopteran
bees, bumblebees
Scaly
winged silkworms
Hemiptera
cochineal
No account yet?
Create an Account